Dental Implants – General Information
Dental Implants are one of the greatest and most revolutionary advancements in dentistry.
Dental Implants are artificial roots that replace missing natural teeth. They transfer the load directly to the jaws, unlike a bridge that relies on remaining teeth to carry the forces.
Dental Implants can be used to:
- Replace individual missing teeth. A dental implant is used to support an artificial crown.
- Replace multiple missing teeth. Two or more dental implants are used to support either individual crowns or a bridge.
- Support and stabilize a partial or full denture.
When dental implants are used to replace missing teeth, the other natural teeth are not involved. They can be placed in most areas of the mouth where teeth are missing. Dental implants can work independently of each other, unlike other types of replacements, which depend on several teeth for support.
The success rate for dental implants is in the 95-99% rate long term. Their success rate is so high that replacement of missing teeth with dental implants has become the treatment of choice in situations that used to involve complex dentistry on questionable teeth.
Dental Implants Case Example 1 – Single Tooth Replacement
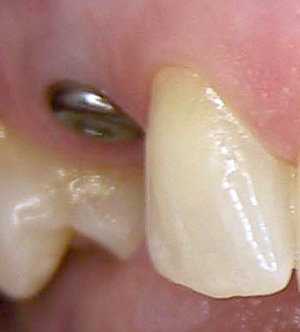
This patient had fractured the root of her upper canine. A dental implant was placed to replace the extracted root. This photo shows the healing abutment in place.
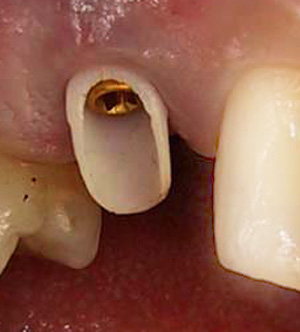
Once the implant had integrated, the healing abutment was replaced with a Zirconium abutment, which was shaped to support the replacement crown.
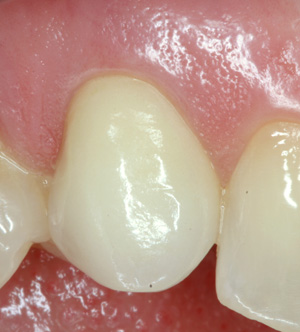
A porcelain crown was cemented over the abutment, restoring her pretty smile.
Dental Implants Case Example 2 – A Bridge on Dental Implants
Dental Implants Case Example 2 – A Bridge on Dental Implants
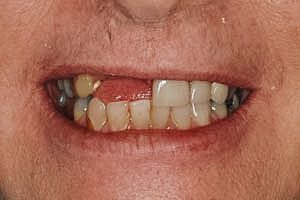
This patient was referred to me for dental implants. She had a fractured root on one of her teeth and two other teeth could not be restored.
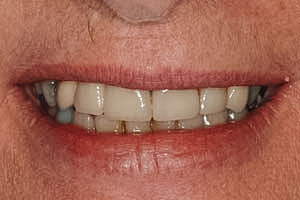
I placed two implants that are supporting a three-unit bridge. She now has her smile restored and has avoided the need for a denture.
Dental Implants – FAQ
Dental Implants – FAQ
Need more information?
For more information about our dental practice in general, or if you have a specific question about your dental care needs, please call us on (02) 8883 4560, email our dental practice at [email protected] or send us a message below and we will do our best to help you.
How can our dental practice help you with your dental care needs?
Whether your dental care needs are a regular dental check-up or you require more comprehensive dental care, the team at our dental practice will do our best to provide you with the best possible advice and care.
Want more information about our dental practice?
For more information about our dental practice in general, or if you have a specific question about your dental care needs, please call us on (02) 8883 4560, email our dental practice at [email protected] or send us a message below and we will do our best to help you.



